A continued partnership with UHC Sainte-Justine for the acquisition of a Monteris NeuroBlate MRI System neurosurgical laser
Kurling for Kids is in its FINAL(!) year for the long-term funding (contribution of $600,000 over four years) of a new, state-of-the-art neurosurgical laser called the Monteris NeuroBlate MRI System. UHC Sainte-Justine is the first pediatric hospital in Canada to acquire this state-of-the-art piece of equipment that will provide multiple added benefits to children.
What’s so exciting about this technology?
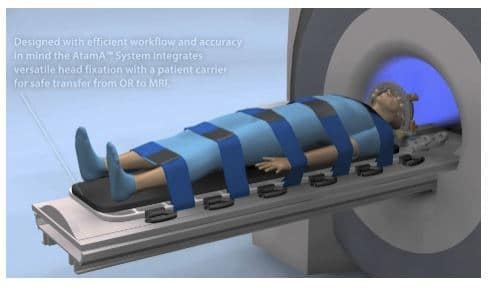
The NeuroBlate System employs diode laser energy delivered via a gas-cooled fiber-optic probe, which allows safe targeting and selective ablation of soft tissue and lesions in the brain, including some that may have traditionally been deemed “inoperable”. It is the only system that monitors ablation contours in 3-Dimensions and provides real-time imaging to support a surgeon’s clinical decision matrix. This allows to operate the brain without touching the unaffected areas surrounding the epileptic lesion or tumor and thus, protects the neurodevelopment of the child, which is the main mission of the Integrated Center Network in Neurodevelopment of the Child (CIRENE).
In other words, the device allows a neurosurgeon to see the tumor live on the magnetic resonance imaging (MRI) of the brain. The neurosurgeon can therefore better see the ablation and use the targeted laser to limit the tissue destruction to the minimum.
To oversee the use of this new technology, the UHC Sainte-Justine has hired Dr. Alexander Weil who is currently the only Canadian pediatric neurosurgeon trained to use this technique. After studying medicine at the University of Sherbrooke, Dr. Weil did his residency at the University of Montreal, then a fellow at the Miami Children’s Hospital (University of Miami) in pediatric neurosurgery and a fellowship in neuro-oncology McGill.
This cutting-edge technology provides several key benefits:
 Minimal invasive technique, which results in shorter hospital stays, less pain medication, faster recovery, minimal scarring, and a superior cosmetic result. Indeed, after 24-48 hours, the child can go home and resume normal activities, contrary to conventional surgery where hospitalization could last between 5 and 14 days, and restrictions in activities, one to two months.
Minimal invasive technique, which results in shorter hospital stays, less pain medication, faster recovery, minimal scarring, and a superior cosmetic result. Indeed, after 24-48 hours, the child can go home and resume normal activities, contrary to conventional surgery where hospitalization could last between 5 and 14 days, and restrictions in activities, one to two months.
- Major savings for our health system since patients no longer need to be admitted to intensive care.
- Greater access to areas of the brain.
- Larger pool of young patients who can benefit from this technique such as children with epilepsy resistant to medical treatment and children with tumors that are difficult to access by conventional surgery
- Patients with epileptic lesions who could not benefit from conventional surgery may now be treated by laser.
Each year, more than 800 patients visit the neurosurgery department of UHC Sainte-Justine and among these, between 200 and 250 patients are operated on. The Neurosurgery Department provides diagnosis, treatment and follow-up for patients aged 0 to 18 years with brain tumors, bone marrow tumors, cysts in the brain or spinal cord, head trauma or hydrocephalus.
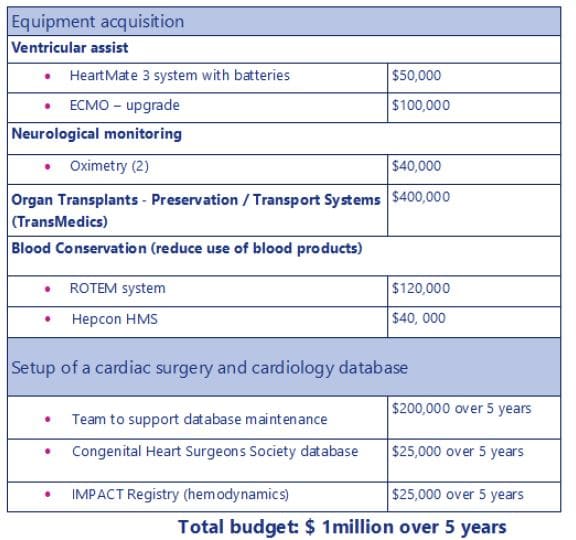
A renewed partnership with UHC Sainte-Justine for the creation of a Center for Pediatric Cardiac Sciences
Sainte-Justine UHC has asked Kurling for Kids to commit for the long-term funding (contribution of $1,000,000 over five years) to create the Pediatric Cardiac Sciences Centre, a true multidisciplinary centre characterized by a joint collaboration of their cardiology, heart surgery, pediatric ICU and neonatal teams.
The centre will make it possible to:
- Centralize the expertise and services available through various groups to provide the highest-quality patient care
- Increase and improve patient access to the hospital’s operating facilities
- Improve access to medical care for patients with rare heart conditions
- Enhance the quality of care for patients using cardiac assist devices and/or waiting for heart transplants
- Improve treatments for congestive heart failure and introduce new mechanical assist devices
- Develop new organ donor strategies (e.g., ex vivo preservation)
- Develop and incorporate blood conservation strategies
- Advance cardiology and heart surgery research, including neurodevelopment
- Team up with various departments at Sainte-Justine and, potentially, the MUHC to combine teams’ strengths and foster synergies
- Develop international cooperation projects.
A centre of this nature would not only improve the quality of care provided to every child, but it would also make it possible to treat more young cardiology and heart surgery patients, cut down on wait times for elective (non-urgent or postponable) procedures, help Sainte-Justine fulfill its duties as a teaching hospital and further strengthen its national and international reputation.